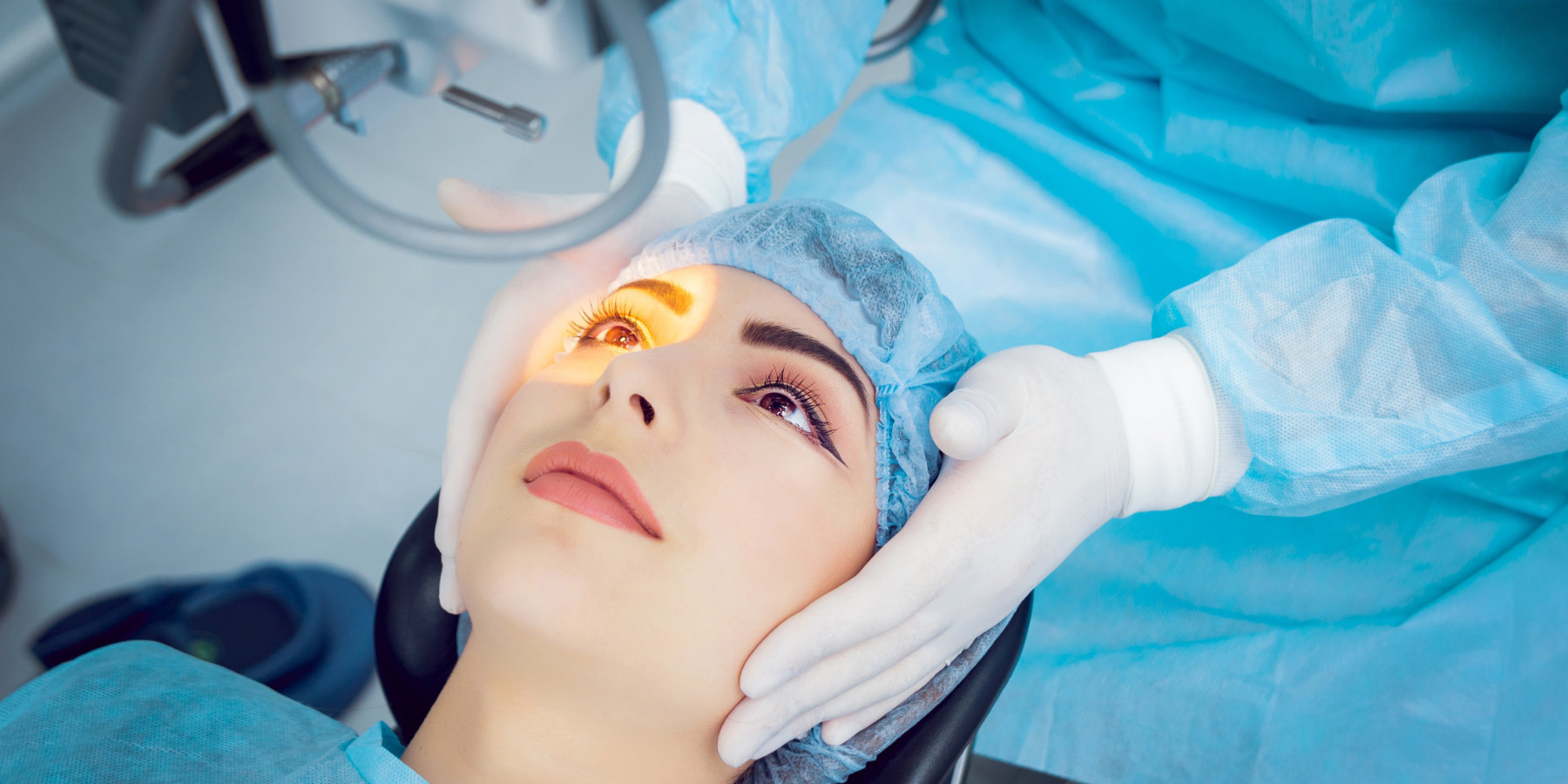
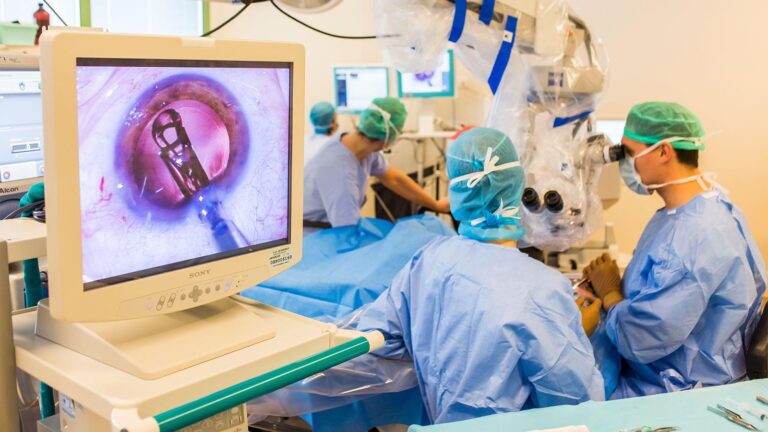
Cataract surgery is the most frequently done surgery globally. While the majority of surgeries are successful, the sheer frequency of procedures increases the possibility that any surgeon may sometimes encounter an unpleasant surprise. With this in mind, three professional surgeons provide advice on how to overcome some of the obstacles that a cataract surgeon may face—and, when possible, how to avoid them entirely.
Planning Ahead
Clearly, the optimal technique for resolving intraoperative complications during cataract surgery consists of two steps:
Reduce the likelihood of an occurrence first, and then be prepared in the case of a setback. In that vein, Audrey R. Talley Rostov, MD, a Seattle-based cornea, cataract, and refractive surgeon, provides the following advice.
• As much as possible, anticipate issues. “There are several strategies for anticipating such complications ahead of cataract surgery,” Dr. Rostov remarks. “First and foremost, if you foresee a more difficult case than typical, one that you do not encounter regularly, such as a sutured IOL, consult with your colleagues in advance about the cataract surgery technique.
“Second, recognize when specialist equipment should be used to prevent a complication during cataract surgery,” she continues. “For example, a very young child’s capsule is substantially more elastic, making capsulorhexis much more difficult. If you have access to a femtosecond laser for capsulorhexis, this may be a suitable application.”
Third, maintain a stock of specialist devices,” she advises. “If the patient is in his or her 90s or extremely young, has a rock-hard nucleus or traumatic cataract, or has a suspected or obvious zonular dehiscence or dialysis, you want to be prepared to deal with cataract surgery complications.”
For example, if a patient has an advanced, thick, white, or brown cataract, I want Malyugin rings, iris hooks, Trypan blue, intraoperative epinephrine, and vitrectomy equipment available in the room in case of an emergency. Obviously, they are not necessary for every situation, but having the equipment on hand avoids the need for your OR team to go looking for it.
“Fourth, have a backup lens on hand in case the bag or the zonules fail,” she recommends. “While this is not a common occurrence following cataract surgery, it is something to anticipate. The STAAR AQ2010 is arguably the best sulcus lens since it has a 13.5 mm focal length rather than a 13 mm focus length. As a backup, have a three-piece IOL on hand; they may be used in the sulcus as long as you understand their limitations. By now, hopefully, every surgeon understands that a single-piece acrylic intraocular lens should never be implanted in the sulcus.”
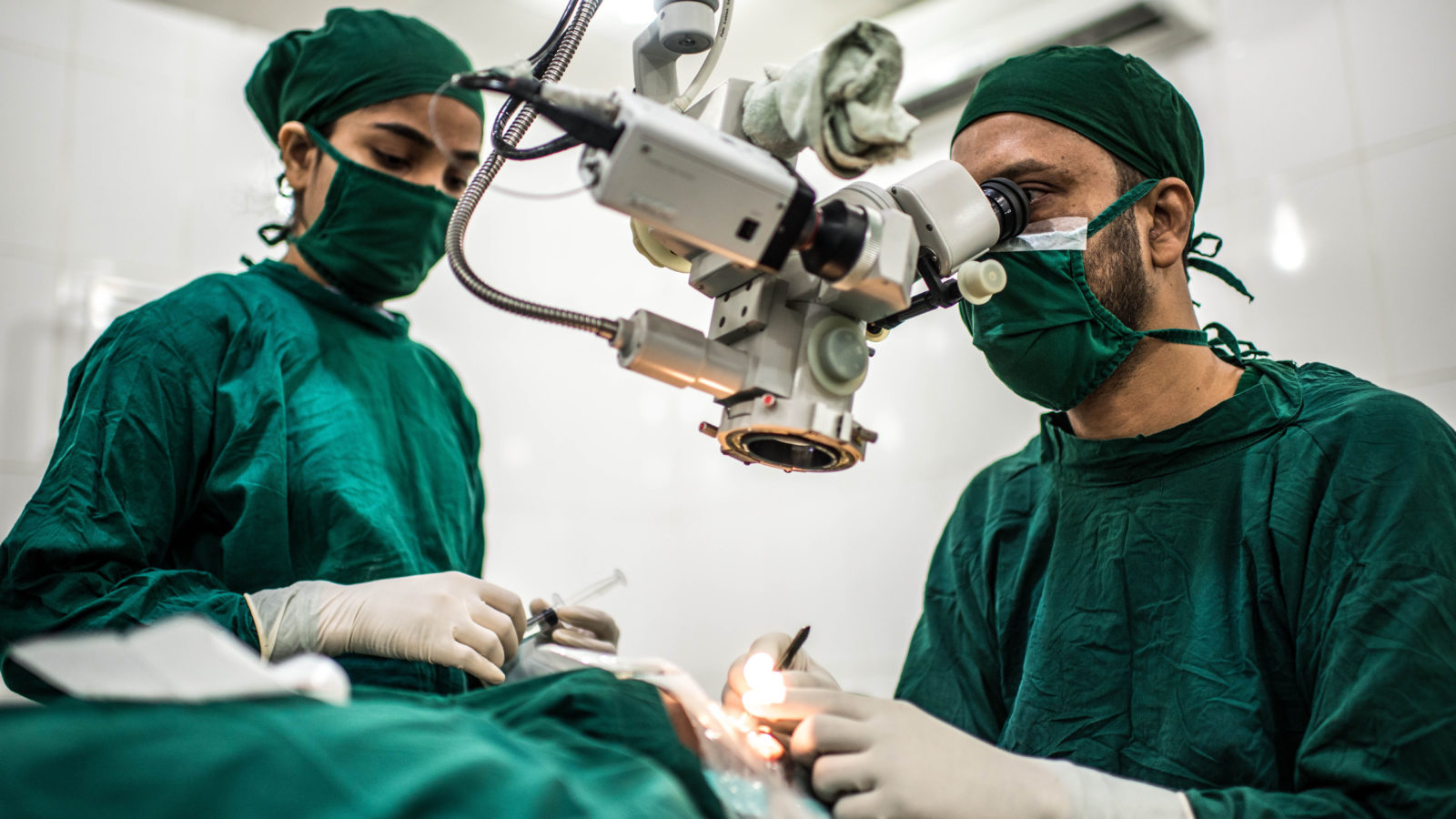
When presented with difficulty, use other strategies. “If standard therapy is pursued in an uncommon context, complications may emerge,” Dr. Rostov advises. “For example, phaco chop may provide complications if the nucleus is very thick and adhered to the capsule. In this scenario, I sculpt extensively and make a gigantic bowl that will ultimately collapse on itself. I may then use viscoelastic to viscodissect it from the posterior capsule. This significantly reduces the likelihood of problems.”
Ensure that your vision is not obstructed. “At times, when the assistant is squirting BSS on the cornea, your sight may be briefly impaired,” Dr. Rostov explains. “You run the danger of facing the capsule, puncturing the posterior capsule, or grabbing the anterior capsule during that short obliteration of your vision. The strategy is to guarantee that your assistance irrigates just briefly and at your explicit request. Then you’ll know when to anticipate it and your viewpoint won’t be blurred at inopportune times, such as during a key move.”
· Be vigilant for warning signs. “Whenever anything unusual happens, stop for a moment,” she suggests. “Be mindful of your surroundings and take a peek around. This is particularly crucial in non-routine situations or ones that may grow more problematic.”
Cornea Complications
With the increasing use of clean corneal incisions in modern cataract surgery, a variety of corneal issues are conceivable.
Corneal abrasions
Corneal abrasions may develop as a result of the wound healing process or as a result of a tool sliding across the eye, such as while inserting the speculum,” notes Robert Weinstock, MD, director of cataract and refractive a cataract surgery at the Eye Institute of West Florida in Largo, Fla. “Almost every instrument used in cataract surgery has the potential to induce an epithelium abrasion, and in certain situations, an epithelial abrasion may impair the surgeon’s vision throughout the process,” he notes. “One method is to coat the cornea with a cohesive viscoelastic to improve surgical visibility and disguise the abrasion. Another option is to debride the central epithelium; however, this is often reserved as a last resort and is done only when visibility inside the eye is considerably limited owing to a cloudy or damaged epithelium.
“At the conclusion of the case, I recommend that a soft contact lens be placed on the eye to relieve acute pain and encourage recovery,” he explains.
Wound burns.
While wound burn is becoming less common these days as a result of improved phaco power modulation and laser cataract softening, it is still possible if a particularly thick nuclear fragment becomes lodged in the phaco needle handpiece or tubing and prevents aspiration passage out of the eye,” Dr. Weinstock explains. “If you are at foot position three and there is no fluid flowing from the eye through the needle, the eye will heat up enough to cause thermal harm to the cornea. If this happens, the ramifications may be very serious.
“Something must be impeding the phaco needle, handpiece, or tubing to cause this sequence of events,” he explains. “A clog may be generated by a thick dispersive viscoelastic or a nucleus particle on rare occasions. If you step on the phaco pedal while a clog prevents fluid from chilling the phaco needle from flowing, you run the danger of getting a wound burn, even if you’re using a brand-new phaco machine with pulse modes. Typically, there are some indicators that anything is wrong; for example, you may detect plumes of white smoke rising from the anterior chamber and nothing emptying from the eye through the phaco needle. Additionally, you’ll likely observe that the cornea becomes yellowish and coagulated, most often on the incision’s front lip. Once you see this, the game is often done.
“Immediately discontinue operations if you find a clog or impediment,” he says. “Remove the phaco needle from the eye and sterile water the tip, handpiece, and tubing. Almost often, I find that the culprit is a large nucleus trapped in the tube.
See Also: Observe these do’s and don’ts after your cataract surgery.